As long as the womb is present fibroids have the potential to regrow. This is because fibroids can develop from a single muscle within the womb and the womb itself is made up of many muscles. Scientific regrowth rates can be up to 40%.
Risk factors for regrowth are:
· Age at which the first operation for fibroids was performed
· The number of fibroids removed: the more fibroids removed the more the likelihood of regrowth.
· When substances like GnRH analogues are used before surgery there is a greater likelihood of regrowth.
Fibroids can be responsible for heavy problems and problems with fertility. And for women who want to be pregnant in the future, the diagnosis of fibroids is a wake up call to embark on trying to get pregnant sooner rather than later. The magic age is 35 years, after which the ovaries, which are responsible for producing eggs, start to decline in function.
After the first operation if fertility is an issue women are thus advised to get on and get pregnant as once their families are complete other methods sometimes more permanent can be used to treat their fibroids.
Treatment options would thus be
1. Hysterectomy: this option would be for women who remain symptomatic after completing their families. The advantage is that once the womb is removed there is no risk of regrowth of fibroids
a. Women may opt to have a subtotal hysterectomy. There have only been 2 reports in literature of fibroid regrowth from the stump of the cervix left behind.
Not all women are comfortable with hysterectomy thus other options would be
2. To continue with medication or Mirena IUS if appropriate
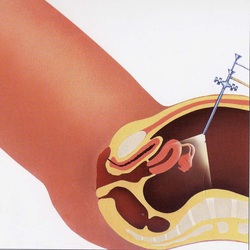
3. Uterine Artery embolization: this is where through the groin area particles are passed to the blood supply of the uterus to block off the blood supply in order to shrink the fibroids
a. It relieves symptoms in 80-90% of women who have it
b. It reduces the size of fibroids by 40-60%
i. Women need to know that maximal effect may take up to a year
c. It is not advised for women who want to get pregnant but women are known to have achieved pregnancy after embolization
d. There is a risk that the ovaries may stop working as a result of the procedure. This happens to 1% of women under the age of 45years after this age the risk increases to about 5%
e. Women who do get pregnant after embolization have a risk of
i. Miscarriage
ii. Caesarean section
iii. Small for dates babies
iv. Malpresentation
v. Post partum Haemorrhage
These complications are for women who have had only an embolization as the primary procedure.
There are no scientific studies for women who have had a myomectomy followed by an embolization who desire pregnancy. One could extrapolate that these complications would be more severe and that the chances of pregnancy would be much less.
There is a recent study that shows that embolization is less successful in women who have had previous myomectomy.
4. Repeat myomectomy:
This of course is an option though the results are much worse for women seeking pregnancy. If they have not been able to achieve pregnancy after the first operation.
· It is a bloodier operation
· The presence of adhesions from the first operation will make the operation more difficult
· There is an increase risk of bowel injury
o After which some women will require a colostomy
· There will be more adhesions
Even for the treatment of symptoms of bleeding a repeat procedure is less successful than the first.
In summary after a first myomectomy if symptoms recur the best treatment is often a hysterectomy. For women who do not want to have a hysterectomy or have not completed their family any other treatment listed above is the next best thing









 RSS Feed
RSS Feed